CRNAs play a crucial role in the health-care profession, and there are numerous benefits to the occupation. But there are also many challenges that CRNAs face in their profession. Current issues like burnout, staffing shortages, and training barriers are some of the responsibilities nurse practitioners face in their practice.
In our guide, we’ll take a closer look at the CRNA role, the responsibilities, what it takes to become one, and the current and future problems.
What Is a CRNA?
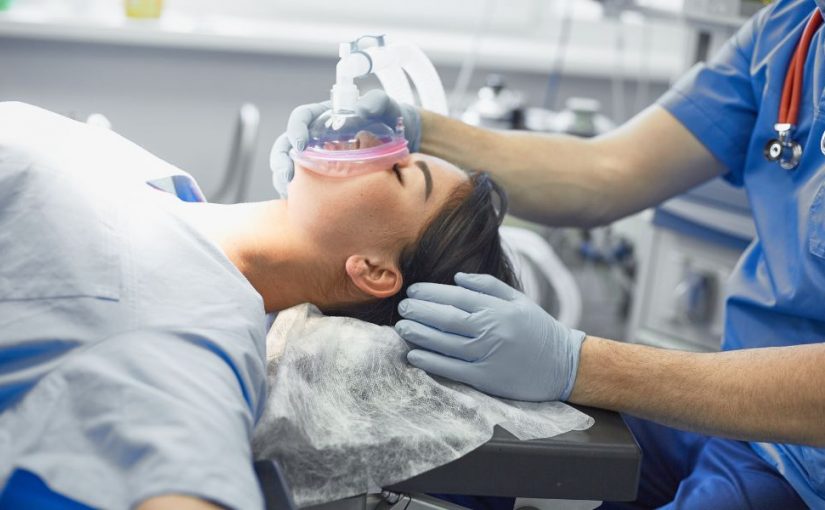
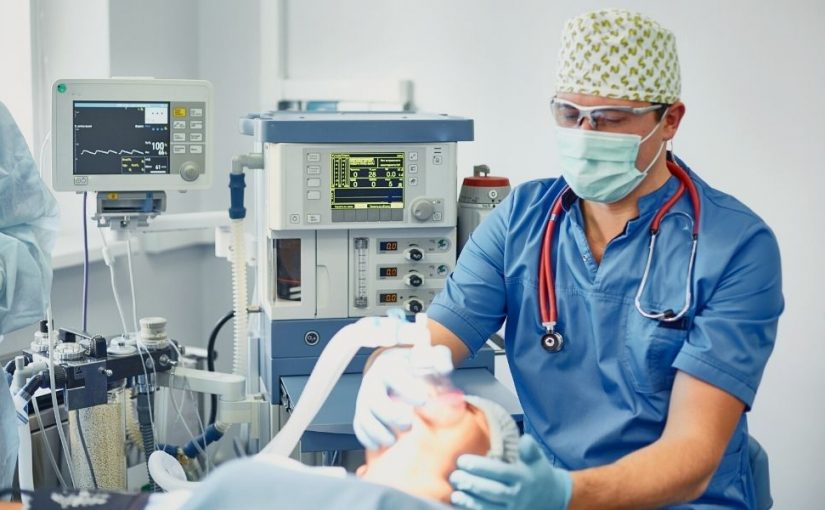
A Certified Registered Nurse Anesthetist (CRNA) has an essential job in anesthesiology. Surgeons and physicians administer anesthesia to a patient through intravenous drugs or inhaled gasses before performing surgery or a medical procedure so that they don’t feel pain.
The CRNA works with the anesthesiologist throughout the procedure. Some of the tasks a CRNA will do include:
- Developing an anesthesia plan
- Educating the patient on the anesthesia plan and procedure
- Physically assessing the patient
- Preparing the patient for the procedure
- Assisting in the administration of the anesthesia
- Supporting, positioning, and monitoring the patient during the procedure
- Monitoring the patient post-procedure
As you can see, a CRNA has many serious responsibilities that will determine the well-being of the patient and the result of the surgery or medical procedure. While an anesthesiologist may develop a big-picture treatment plan for many patients, the CRNA is responsible for the daily tasks and monitoring of patients.
Where Do CRNAs Work?
CRNAs can work in any health-care facility that performs medical procedures or surgeries requiring local or general anesthesia. CRNAs work in:
- Hospitals
- Surgical clinics
- Outpatient care centers
- Doctor’s offices
- Emergency rooms
- Military facilities
How Do You Become a CRNA?
Joining the CRNA profession is a long and challenging process that can take nearly a decade of schooling, training, and working. First, an individual must become a Registered Nurse (RN) before becoming a CRNA.
Therefore, they must first obtain a degree in nursing or an associate degree and pass the National Council Licensure Exam to get an RN license. It typically takes two to four years for an individual to begin schooling and eventually obtain an RN license.
Once licensed, an RN will work to gain experience, typically for about a year, before entering a postgraduate nursing program. A CRNA postgraduate program will usually take two to three years, although some accelerated curriculums are faster by a few months.
After years of courses and clinicals, the individual can take the certifications exam from the National Board of Certification and Recertification for Nurse Anesthetists. Once passed, they receive their license.
The Benefits of Becoming a CRNA
As anyone can see, it takes a lot of commitment to become a CNRA, so what are the benefits of joining the profession? CRNAs are a growing career, and industry experts expect the demand for their skills and training to grow in the coming years.
Good Wages
There’s no doubt that some choose the CRNA profession because it’s one of the best-paying nursing jobs available. Various factors affect individual wages, but the median salary in the profession is around $180,000.
In more rural states and areas, like Wyoming or Idaho, demand is high for CRNAs, so the salary increases even more. The top wage for CRNAs hovers around $270,000 a year, so there’s a payoff for those years of school and training.
In Demand
The anesthesiology field already has a strong demand for capable and effective CRNAs, and industry experts predict that demand will continue to increase in the coming years. The US is an aging population, which means there’ll be a more significant proportion of older people in the coming years.
An aging population means more chronic conditions and comorbidities—ailments that require more surgical procedures and anesthesia. Over the next decade, CRNAs will be one of the most in-demand jobs in the health-care industry, which will lead to higher wages and better benefits.
Autonomy
Although CRNAs work hand-in-hand with anesthesiologists, they enjoy a lot of autonomy in their daily tasks and responsibilities. They don’t do their job with a supervisor breathing down their neck all day— they perform the bulk of the work on their own in many cases.
Many CRNAs say that one of their favorite parts of the job is the leeway they have to make decisions about treatment and patient monitoring. But is being a CRNA stressful? Like most health care professions, it is more physically and emotionally demanding than many other jobs.
6 Challenges CRNAs Face
It’s not all positive for CRNAs, though. There are still many challenges that CRNAs face in their profession, from staffing shortages to education barriers and more.
Burnout
CRNA burnout is real, and it’s perhaps the biggest challenge that CRNAs face is the mental and physical fatigue from the job. Burnout is not exclusively a CRNA problem—the entire medical profession deals with this dilemma, which the COVID-19 pandemic worsened.
According to the American Association of Nurse Anesthesiology, four out of every 10 CRNAs reported high levels of occupational burnout during the pandemic. Burnout amongst CRNAs means that more people are likely to change careers, retire, or make mistakes on the job due to physical or mental fatigue. The causes of burnout varies, but one culprit is a CRNA shortage.
Nurse Shortage
One of the principal reasons for burnout amongst CRNAs and the entire industry is the nursing shortage. A shortage of nurses was a problem for many areas of the health-care industry before the pandemic, and COVID-19 exacerbated the challenge.
Over the next decade, the health-care industry expects to have a shortage of nurses in numerous professions, including CRNAs. More nurses are leaving voluntarily or retiring, and because the education and training of CRNAs is such a long and arduous process, many people worry that there won’t be enough trained professionals to fill the gaps left open.
Increase Demand
While this shortage is occurring, there’s also an increase in demand for CRNAs. Many rural or impoverished communities are trying to expand their health-care capabilities, and CRNAs play an essential role.
But are there enough CRNAs to fill these roles? That’s one of the significant challenges facing the profession in the next decade.
Education and Training Barriers
As we laid out, it takes many years of schooling and training for an individual to become a CRNA. They have many crucial responsibilities, so education is necessary, but it presents a considerable barrier to growing the profession. After all, many people don’t have the time or money to spend six or eight years working toward becoming a CRNA.
Significant Responsibilities
Every day, a CRNA works with patients that could be facing life-or-death circumstances, depending on the setting and the medical procedure. Anesthesia can present many severe problems to a patient’s health if there are mistakes, which is why CRNAs and anesthesiologists undergo so much training and education. But it’s no doubt a challenge for CRNAs to have such drastic responsibility almost every day at work.
Malpractice Lawsuits
Nobody, not even a CRNA, is perfect. In fact, the issues nurse practitioners face happen in most other health care professions. CRNAs make mistakes like everyone else, but when errors happen, they can result in dire consequences, leading to malpractice lawsuits. Everyone working in the medical profession has to deal with malpractice claims, and CRNAs are no different.
That’s why CRNA liability insurance is necessary for all CRNAs to protect their careers and financial lives. Liability coverage ensures that CRNAs have a fair chance and won’t lose their career over a mistake. Contact us for a quote regarding malpractice insurance. To learn more about CRNA burnout, shortage, and other challenges, explore our blogs.